Genetic testing in cancer evaluates inherited (germline) mutations that may influence both treatment decisions and long-term risk assessment. It helps identify individuals at increased lifetime cancer risk and guides preventive strategies, screening intensity, and in some cases, targeted therapy selection. Not every patient requires genetic testing, but when appropriately indicated, it significantly alters clinical management for both patients and families.
In clinical oncology practice, interpreting genetic results requires structured evaluation — balancing risk prediction, treatment relevance, and family implications.
Germline genetic testing informs both cancer treatment decisions and preventive risk management.
What Is the Difference Between Germline and Tumor Genetic Testing?
Understanding the distinction is foundational.
- Germline testing: Identifies inherited mutations present in every cell of the body.
- Tumor testing: Detects mutations acquired within cancer cells.
- Germline results affect family members; tumor results primarily guide treatment.
Both are important, but they answer different clinical questions.
When Should Genetic Testing Be Considered?
Testing is recommended based on structured risk indicators rather than routine screening for all patients.
- Early age of cancer diagnosis.
- Multiple primary cancers in the same individual.
- Strong family history of related cancers.
- Specific tumor types known for hereditary syndromes.
- Guideline-based indications (e.g., breast, ovarian, colorectal cancers).
Risk assessment models and pedigree analysis often precede testing decisions.
How Does Genetic Testing Influence Treatment?
In certain cancers, inherited mutations directly influence therapeutic selection.
- If BRCA mutation present → PARP inhibitor eligibility may be considered.
- If Lynch syndrome identified → Immunotherapy sensitivity may be relevant.
- If high-risk mutation found → Prophylactic surgical strategies may be discussed.
- If no pathogenic mutation detected → Standard management continues.
Importantly, interpretation requires clinical correlation — not every mutation changes management.
What Is the Structured Decision Logic for Hereditary Risk Assessment?
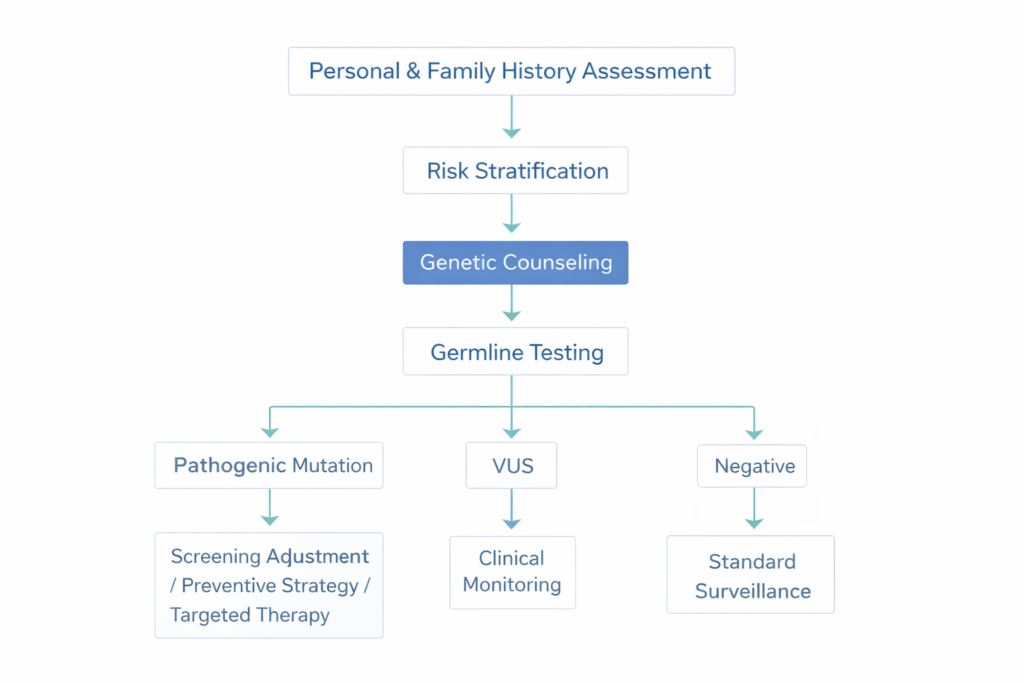
Hereditary cancer risk decision-tree.
Why Is Genetic Counseling Essential?
Genetic information has psychological, familial, and ethical implications. Structured counseling ensures appropriate consent, interpretation, and communication.
- Avoids misinterpretation of variants.
- Prevents unnecessary anxiety.
- Ensures cascade testing for family members when appropriate.
Where Does a Second Opinion Add Value?
Complex genetic reports can contain variants of uncertain significance or ambiguous recommendations. A structured second review helps confirm whether findings truly alter treatment or preventive strategy.
FAQ: Genetic Testing in Cancer
Does everyone with cancer need genetic testing?
No. Testing depends on tumor type, age, family history, and guideline criteria.
Will a positive result mean my children will develop cancer?
A positive mutation increases risk but does not guarantee cancer development.
What is a Variant of Uncertain Significance (VUS)?
A VUS is a genetic change whose clinical impact is not yet clearly established.
Can genetic testing prevent cancer?
It does not prevent cancer directly but enables risk-reducing strategies and earlier detection.
Is genetic testing confidential?
Testing is conducted under medical confidentiality and ethical standards.
Related Articles
How Structured Second Opinions Improve Cancer Treatment Decisions
Genetic testing for successful cancer treatment
Closing Perspective
Genetic testing in oncology bridges treatment precision and preventive strategy. When appropriately applied, it protects not only the patient but potentially generations within a family. Clinical rigor, not routine testing, remains the guiding principle.
Educational Disclaimer: This article is for educational purposes only and does not replace individualized medical advice. Genetic testing decisions should be made in consultation with a qualified oncology specialist and genetic counselor.
Pingback: Biomarker-Driven Therapy in Modern Oncology
Pingback: Precision oncology integrates molecular profiling with